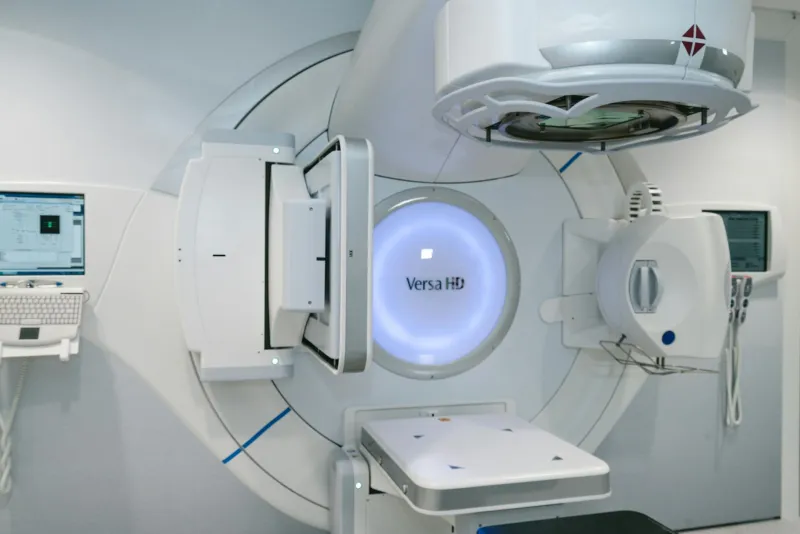
The Invisible Infrastructure of Modern Medicine
Every Tuesday morning, a refrigerated lorry crosses the Channel carrying cargo worth more than gold: medical radioisotopes with half-lives measured in hours. These radioactive materials enable the PET scans that detect early-stage cancers, the therapeutic doses that shrink tumours, and the diagnostic procedures that guide surgical interventions across Britain's healthcare system.
Yet this critical supply chain operates on a knife's edge, dependent on a handful of ageing nuclear reactors in Belgium, the Netherlands, and Canada. When these facilities experience unplanned shutdowns—as they increasingly do—NHS nuclear medicine departments face impossible choices between rationing life-saving treatments and depleting emergency reserves.
"We're essentially flying blind," explains Dr Catherine Walsh, nuclear medicine consultant at Guy's and St Thomas' Hospital. "One reactor failure in Belgium can force us to cancel cancer treatments across London within 48 hours."
 Photo: Guy's and St Thomas' Hospital, via www.tagvenue.com
Photo: Guy's and St Thomas' Hospital, via www.tagvenue.com
The Physics of Vulnerability
Medical radioisotopes present unique logistical challenges that distinguish them from conventional pharmaceuticals. Technetium-99m, the workhorse of nuclear medicine, has a half-life of six hours—meaning half the material becomes useless every six hours regardless of storage conditions. Fluorine-18, essential for PET scanning, degrades even faster with a two-hour half-life.
This decay schedule means isotopes must be produced continuously and delivered with precision timing. A delayed shipment doesn't just reduce available supply—it can render entire batches worthless by the time they reach patients.
Britain currently imports approximately 95% of its medical radioisotopes, primarily from the High Flux Reactor in the Netherlands and the BR2 reactor in Belgium. Both facilities began operation in the 1960s and now require increasingly frequent maintenance shutdowns that disrupt global supply chains.
 Photo: High Flux Reactor, via c8.alamy.com
Photo: High Flux Reactor, via c8.alamy.com
Recent Crisis Points
The fragility of this system became apparent during several high-profile disruptions over the past five years. In 2018, the simultaneous shutdown of both major European reactors forced NHS trusts to postpone thousands of diagnostic procedures and cancer treatments.
During a 2021 supply crisis, nuclear medicine departments implemented emergency protocols that prioritised urgent cancer cases while deferring routine cardiac imaging. Some hospitals chartered private aircraft to transport isotopes from Canadian suppliers, at costs exceeding £50,000 per flight.
"We had patients with suspected heart attacks waiting three days for stress tests because we couldn't get technetium," recalls Dr Michael Chen, nuclear medicine physician at Manchester University NHS Foundation Trust. "These weren't scheduling preferences—they were clinical emergencies."
The Economic Calculus
Beyond immediate patient care impacts, supply disruptions impose significant financial costs on NHS trusts. Nuclear medicine departments must maintain expensive equipment and trained staff even when isotope shortages prevent normal operations. Private healthcare providers often outbid NHS trusts for limited supplies during crises, further restricting public sector access.
The Royal College of Radiologists estimates that isotope supply disruptions cost the NHS approximately £15 million annually in cancelled procedures, emergency procurement, and delayed diagnoses that require more expensive interventions later.
These calculations exclude the broader economic impact of delayed cancer diagnoses, which the Macmillan Cancer Support charity suggests may cost the healthcare system hundreds of millions in additional treatment expenses over patients' lifetimes.
Domestic Production Possibilities
Several British institutions possess the technical capability to produce medical radioisotopes but lack the regulatory approval and financial investment necessary for commercial operation. The University of Birmingham's cyclotron facility produces research quantities of various isotopes, while the Dalton Cumbrian Facility has explored domestic molybdenum-99 production.
 Photo: University of Birmingham, via birmingham.autism-uni.org
Photo: University of Birmingham, via birmingham.autism-uni.org
However, establishing reliable domestic production requires substantial upfront investment that successive governments have been reluctant to provide. Building a medical isotope reactor costs approximately £200-300 million, with additional regulatory compliance expenses that can extend development timelines by decades.
"The business case is challenging because isotopes decay so quickly," explains Professor David Parker, radiochemist at Durham University. "You can't stockpile them like conventional medicines, so domestic production must be economically viable based on immediate demand alone."
Alternative Technologies
Emerging technologies offer potential alternatives to reactor-produced isotopes. Linear accelerators can generate some medical isotopes through different nuclear processes, while new reactor designs promise more reliable operation than current ageing facilities.
Several British companies are developing novel approaches to isotope production. Advanced Accelerator Applications UK is investigating generator systems that could produce radioisotopes on-demand at hospital sites, eliminating transportation delays and decay losses.
However, these technologies remain years away from clinical implementation and require substantial research investment to demonstrate safety and efficacy equivalent to established isotopes.
International Collaboration
Recognising shared vulnerabilities, several European countries are exploring collaborative approaches to isotope security. The European Observatory on Health Systems and Policies has recommended coordinated investment in new production facilities and improved supply chain resilience.
Britain's post-Brexit status complicates participation in such initiatives, though bilateral agreements with individual countries could provide some supply diversification. Recent discussions with Canadian suppliers have explored dedicated production capacity for British healthcare needs, though such arrangements would require long-term financial commitments.
Professional Advocacy
The nuclear medicine community has increasingly vocal about supply chain vulnerabilities. The British Nuclear Medicine Society has called for government intervention to ensure reliable isotope access, while the Society and College of Radiographers has highlighted workforce implications of unpredictable supply disruptions.
"Our staff are highly trained professionals who shouldn't spend their time worrying about whether basic materials will be available tomorrow," argues Dr Walsh. "This uncertainty undermines recruitment and retention in an already specialised field."
Policy Options
Addressing Britain's isotope dependence requires coordinated action across multiple government departments. The Department of Health and Social Care could establish strategic reserves for critical isotopes, while UK Research and Innovation could prioritise funding for domestic production research.
The Nuclear Decommissioning Authority possesses relevant expertise and facilities that could potentially support medical isotope production, though such dual-use arrangements would require careful regulatory oversight.
More immediately, NHS England could develop better contingency planning that coordinates responses to supply disruptions across regional networks, reducing the current system where individual trusts compete for limited supplies during crises.
The Broader Context
Britain's isotope vulnerability reflects broader challenges in maintaining complex healthcare infrastructure. Like other advanced medical technologies, nuclear medicine requires sustained investment and long-term planning that often conflicts with short-term budget pressures.
The COVID-19 pandemic demonstrated how supply chain disruptions can cascade through healthcare systems in unexpected ways. Medical isotopes represent a similar single point of failure that could significantly impact cancer care across Britain if current trends continue.
"We're one major reactor failure away from a genuine crisis," warns Dr Chen. "The question is whether we'll invest in resilience before that happens or after."